Blogs Details
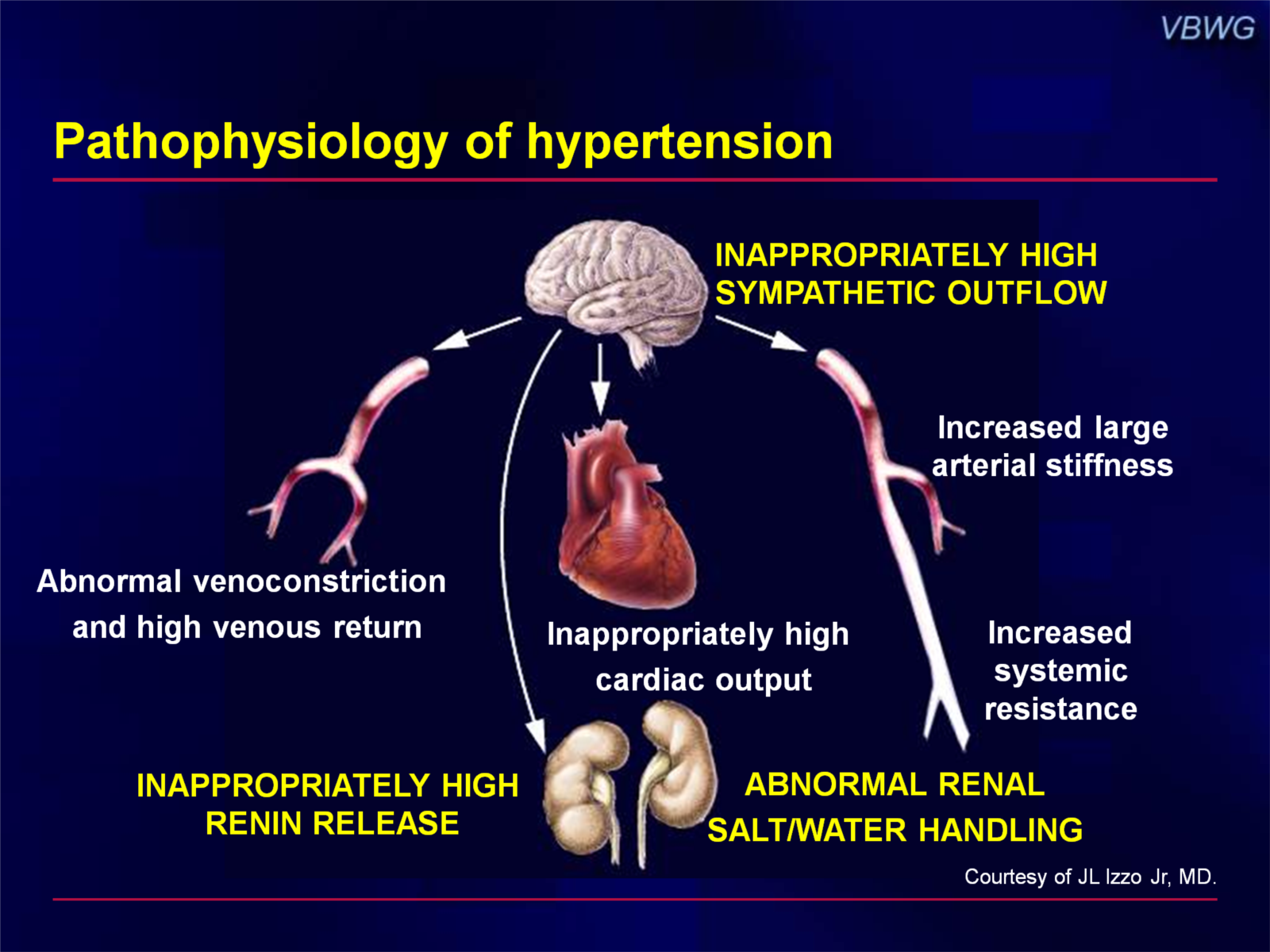
HYPERTENSION
HYPERTENSION-
•Hypertension is sustained elevation of BP
– Systolic blood pressure ³ 140 mm Hg
– Diastolic blood pressure ³ 90 mm Hg
•Primary – 90-95% of cases – also termed “essential” of “idiopathic”
•Secondary – about 5% of cases
–Renal or renovascular disease
–Endocrine disease
•Phaeochomocytoma
•Cusings syndrome
•Conn’s syndrome
•Acromegaly and hypothyroidism
–Coarctation of the aorta
–Iatrogenic
•Hormonal / oral contraceptive
•NSAIDs
HYPERTENSION-]
A systolic blood pressure ( SBP) >139 mmHg and/or
nA diastolic (DBP) >89 mmHg.
nBased on the average of two or more properly measured, seated BP readings.
On each of two or more office visits
Prehypertension
SBP >120 mmHg and <139mmHg and/or
nDBP >80 mmHg and <89 mmHg.
Prehypertension is not a disease category rather a designation for individuals at high risk of developing HTN
Classification of Hypertension
•Primary Hypertension
- Contributing factors:
• SNS activity
• Diabetes mellitus
• Sodium intake
• Excessive alcohol intake
Secondary Hypertension
- Contributing factors:
• Coarctation of aorta
• Renal disease
• Endocrine disorders
• Neurologic disorders
- Rx: Treat underlying cause
Risk Factors for Primary Hypertension
•Age (> 55 for men; > 65 for women)
•Alcohol
•Cigarette smoking
•Diabetes mellitus
•Elevated serum lipids
•Excess dietary sodium
•Gender
•Family history
•Obesity (BMI > 30)
•Ethnicity (African Americans)
•Sedentary lifestyle
•Socioeconomic status
•Stress
Hypertension
Clinical Manifestations
Frequently asymptomatic until severe and target organ disease has occurred
–Fatigue, reduced activity tolerance
–Dizziness
–Palpitations, angina
–Dyspnea
Hypertension: Complications
§Cerebrovascular Disease
• Stroke
§ Peripheral Vascular Disease
§ Nephrosclerosis
§ Retinal Damage
Treatment Goals
•Goal is to reduce overall cardiovascular risk factors and control BP by the least intrusive means possible
–BP < 140/90
–In patients with diabetes or renal disease, goal is < 130/80
Benefits of Lowering BP
Average Percent Reduction
Stroke incidence 35–40%
Myocardial infarction 20–25%
Heart failure 50%
Hypertension
Collaborative Care
Lifestyle Modifications
- Weight reduction
- Dietary changes (DASH diet)
- Limitation of alcohol intake (< 2 drinks/day for men;
< 1/day for women)
- Regular physical activity
- Avoidance of tobacco use
- Stress management
• Nutritional Therapy: DASH Diet = Dietary Approahes to Stop HTN
- Sodium restriction
- Rich in vegetables, fruit, and nonfat
dairy products
- Calorie restriction if overweight
Drug Therapy
- Reduce SVR
- Decrease volume of circulating blood
•Diuretics
•Adrenergic inhibitors
•β - Adrenergic blockers
•ACE Inhibitors
Calcium channel blockers
Hypertension: Drug Therapy
•Thiazide-type Diuretics
–Inhibit NaCl reabsorption
–Side effects:
•Electrolyte imbalances: ↓ Na, ↓ Cl, ↓ K** (advise K rich foods)
•Fluid volume depletion (monitor for orthostatic hypotension)
•Impotence, decreased libido
•Adrenergic Inhibitors
–Reduce sympathetic effects that cause HTN by:
•Reducing sympathetic outflow
•Blocking effects of sympathetic activity on vessels
–Side effects
•Hypotension
• Varied, depending on specific drug
• Drug Therapy and Patient Teaching
- Identify, report, and minimize side effects
• Orthostatic hypotension
• Sexual dysfunction
• Dry mouth
• Frequent urination
Primary Hypertension
Nursing Management
Nursing Diagnoses
Ineffective health maintenance
- Anxiety
- Sexual dysfunction
- Ineffective therapeutic regimen management r/t
- lack of S/S of HTN, side effects of Rx, cost of Rx, etc.
Health Promotion
• Individual patient evaluation
• Screening programs
• Cardiovascular risk factor modification
Hypertensive Crisis
• Severe, abrupt elevation in BP
• The rate of in BP is more important than the absolute value
• Most common in patients with a history of HTN who have failed to comply with medications or who have been under-medicated
Hypertensive Crisis
Clinical Manifestations
- Hypertensive encephalopathy (H/A, N & V,
seizures, confusion, coma)
- Renal insufficiency
- Heart failure
- Pulmonary edema